

Read this text to explore how Western societies have treated people with psychological disorders throughout history. In 1963, the U.S. Congress emptied the nation's mental health institutions or asylums through a process we call deinstitutionalization because the conditions were so tragic and dreadful. Today, we deliver mental health services in community mental health centers, but many of the services they provide are inadequate. Statistics show that 26 percent of homeless adults living in shelters experience mental illness. Many people have been incarcerated because they are in unfortunate circumstances or because members of the community are frightened by the negative effects or anti-social aspects of their illnesses.
Before we explore the various approaches to therapy used today, let's begin our study of therapy by looking at how many people experience mental illness and how many receive treatment. According to the U.S. Department of Health and Human Services (2013), 19 percent of U.S. adults experienced mental illness in 2012. For teens (ages 13–18), the rate is similar to that of adults, and for children ages 8–15, current estimates suggest that 13 percent experience mental illness in a given year (National Institute of Mental Health [NIMH], n.d.-a)
With many different treatment options available, approximately how many people receive mental health treatment per year? According to the Substance Abuse and Mental Health Services Administration (SAMHSA), in 2008, 13.4 percent of adults received treatment for a mental health issue (NIMH, n.d.-b). These percentages, shown in Figure 16.2, reflect the number of adults who received care in inpatient and outpatient settings and/or used prescription medication for psychological disorders.
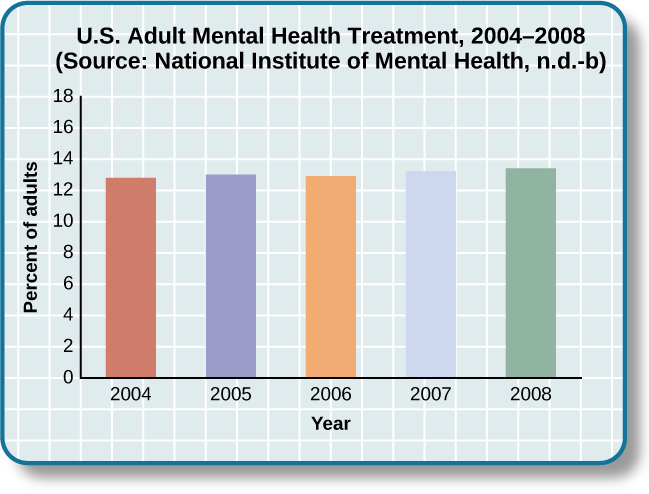
Figure 16.2 The percentage of adults who received mental health treatment in 2004–2008 is shown. Adults seeking treatment increased slightly from 2004 to 2008.
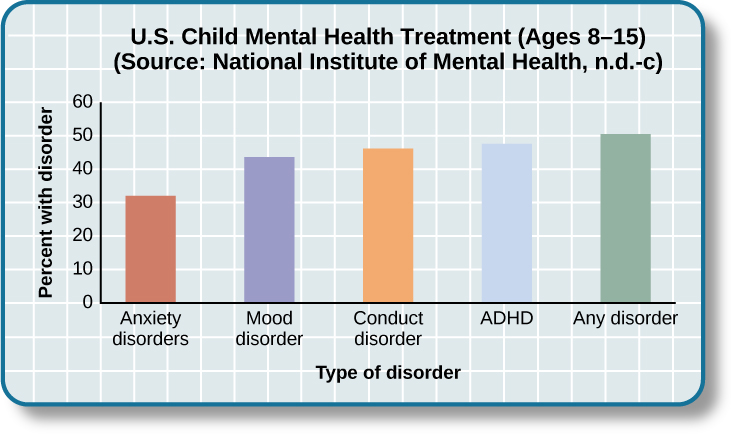
Figure 16.3 About one-third to one-half of U.S. adolescents (ages 8–15) with mental disorders receive treatment, with behavior-related disorders more likely to be treated.
For much of history, the mentally ill have been treated very poorly. It was believed that mental illness was caused by demonic possession, witchcraft, or an angry god. For example, in medieval times, abnormal behaviors were viewed as a sign that a person was possessed by demons. If someone was considered to be possessed, there were several forms of treatment to release spirits from the individual. The most common treatment was exorcism, often conducted by priests or other religious figures: Incantations and prayers were said over the person's body, and she may have been given some medicinal drinks.
Another form of treatment for extreme cases of mental illness was trephining: A small hole was made in the afflicted individual's skull to release spirits from the body. Most people treated in this manner died. In addition to exorcism and trephining, other practices involved execution or imprisonment of people with psychological disorders. Still others were left to be homeless beggars.
Generally speaking, most people who exhibited strange behaviors were greatly misunderstood and treated cruelly. The prevailing theory of psychopathology in earlier history was the idea that mental illness was the result of demonic possession by either an evil spirit or an evil god because early beliefs incorrectly attributed all unexplainable phenomena to deities deemed either good or evil.
From the late 1400s to the late 1600s, a common belief perpetuated by some religious organizations was that some people made pacts with the devil and committed horrible acts, such as eating babies. These people were considered to be witches and were tried and condemned by courts - they were often burned at the stake. Worldwide, it is estimated that tens of thousands of mentally ill people were killed after being accused of being witches or under the influence of witchcraft.
By the 18th century, people who were considered odd and unusual were placed in asylums (Figure 16.4). Asylums were the first institutions created for the specific purpose of housing people with psychological disorders, but the focus was ostracizing them from society rather than treating their disorders. Often these people were kept in windowless dungeons, beaten, chained to their beds, and had little to no contact with caregivers.

Figure 16.4 This painting by Francisco Goya, called The Madhouse, depicts a mental asylum and its inhabitants in the early 1800s. It portrays those with psychological disorders as victims.

Figure 16.5 This painting by Tony Robert-Fleury depicts Dr. Philippe Pinel ordering the removal of chains from patients at the Salpêtrière asylum in Paris.

Figure 16.6 Dorothea Dix was a social reformer who became an advocate for the indigent insane and was instrumental in creating the first American mental asylum. She did this by relentlessly lobbying state legislatures and Congress to set up and fund such institutions.
This legislation changed how mental health services were delivered in the United States. It started the process of deinstitutionalization, the closing of large asylums, by providing for people to stay in their communities and be treated locally. In 1955, there were 558,239 severely mentally ill patients institutionalized at public hospitals. By 1994, by percentage of the population, there were 92 percent fewer hospitalized individuals.
Today, there are community mental health centers across the nation. They are located in neighborhoods near the homes of clients, and they provide large numbers of people with mental health services of various kinds and for many kinds of problems. Unfortunately, part of what occurred with deinstitutionalization was that those released from institutions were supposed to go to newly created centers, but the system was not set up effectively. Centers were underfunded, staff was not trained to handle severe illnesses such as schizophrenia, there was high staff burnout, and no provision was made for the other services people needed, such as housing, food, and job training.
Without these supports, those people released under deinstitutionalization often ended up homeless. Even today, a large portion of the homeless population is considered to be mentally ill (Figure 16.7). Statistics show that 26 percent of homeless adults living in shelters experience mental illness (U.S. Department of Housing and Urban Development [HUD], 2011).

Figure 16.7 (a) Of the homeless individuals in U.S. shelters, about one-quarter have a severe mental illness (HUD, 2011). (b) Correctional institutions also report a high number of individuals living with mental illness. (credit a: modification of work by C.G.P. Grey; credit b: modification of work by Bart Everson)

Figure 16.8 Therapy with children may involve play.
Some people seek therapy because the criminal justice system referred them or required them to go. For some individuals, for example, attending weekly counseling sessions might be a condition of parole. If an individual is mandated to attend therapy, she is seeking services involuntarily. Involuntary treatment refers to therapy that is not the individual's choice. Other individuals might voluntarily seek treatment. Voluntary treatment means the person chooses to attend therapy to obtain relief from symptoms.
Psychological treatment can occur in a variety of places. An individual might go to a community mental health center or a practitioner in private or community practice. A child might see a school counselor, school psychologist, or school social worker. An incarcerated person might receive group therapy in prison. There are many different types of treatment providers, and licensing requirements vary from state to state. Besides psychologists and psychiatrists, there are clinical social workers, marriage and family therapists, and trained religious personnel who also perform counseling and therapy.
A range of funding sources pay for mental health treatment: health insurance, government, and private pay. In the past, even when people had health insurance, the coverage would not always pay for mental health services. This changed with the Mental Health Parity and Addiction Equity Act of 2008, which requires group health plans and insurers to make sure there is parity of mental health services (U.S. Department of Labor, n.d.). This means that co-pays, total number of visits, and deductibles for mental health and substance abuse treatment need to be equal to and cannot be more restrictive or harsher than those for physical illnesses and medical/surgical problems.
Finding treatment sources is also not always easy: there may be limited options, especially in rural areas and low-income urban areas; waiting lists; poor quality of care available for indigent patients; and financial obstacles such as co-pays, deductibles, and time off from work. Over 85 percent of the 1,669 federally designated mental health professional shortage areas are rural; often primary care physicians and law enforcement are the first-line mental health providers, although they do not have the specialized training of a mental health professional, who often would be better equipped to provide care.
Availability, accessibility, and acceptability (the stigma attached to mental illness) are all problems in rural areas. Approximately two-thirds of those with symptoms receive no care at all (U.S. Department of Health and Human Services, 2005; Wagenfeld, Murray, Mohatt, & DeBruiynb, 1994). At the end of 2013, the U.S. Department of Agriculture announced an investment of $50 million to help improve access and treatment for mental health problems as part of the Obama administration's effort to strengthen rural communities.
Source: Rice University, https://openstax.org/books/psychology/pages/16-1-mental-health-treatment-past-and-present
 This work is licensed under a Creative Commons Attribution 4.0 License.
This work is licensed under a Creative Commons Attribution 4.0 License.